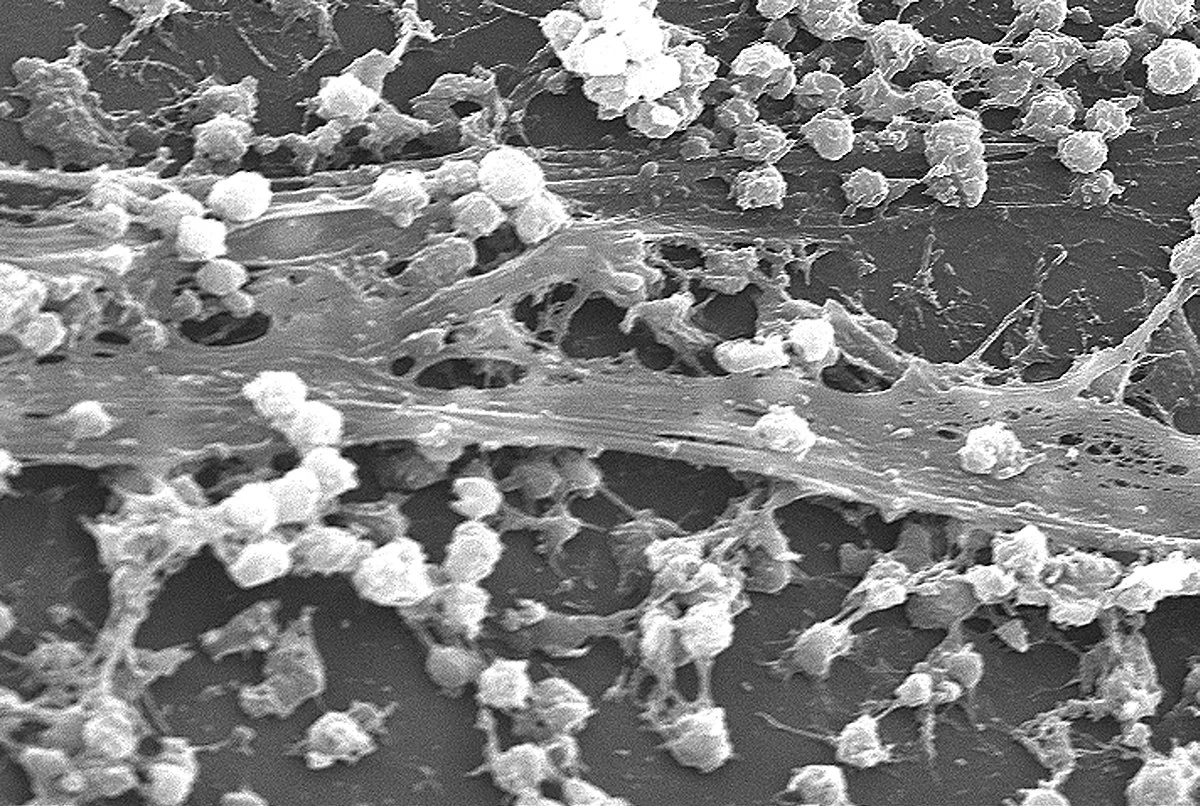
Biofilms And Your Immune Recovery
Many of us carry the illusion that with the aid of antibiotics or antifungal medications, our bodies are able to seek and destroy pathogens in the body simply and effectively. However, most bacteria and fungi, in particular, exist inside of communities called biofilms. To form a biofilm, bacteria first use specific mechanisms to adhere to a surface and then construct a matrix that also sequesters calcium, magnesium, iron, or whatever minerals are available. Since the pathogens are unselective about materials used, heavy metals may also come into play in this process.
The National Institutes of Health (NIH) revealed that among all microbial and chronic infections, 65% and 80%, respectively, are associated with biofilm formation.
Tucked inside a biofilm, bacteria and/or fungi share nutrients and host DNA. They also undergo changes to evade the immune system. Biofilm is a hostile community for most antibiotics. This hostility is created by down-regulating the metabolic activity of their "core" bacteria, decreasing the oxygen concentration and altering the pH at their core (1). In addition, the biofilm forms a physical barrier that prevents immune cells from detecting the pathogens. According to the National Institutes of Health (NIH), more than 80% of our current bacterial infections involve biofilm (2). This means that standard forms of treatment are potentially ineffective 80% of the time, as they are designed/targeted for free-floating planktonic-type pathogens.
The digestive tract is a prime location for biofilm development. It has huge surface area and continual influx of nutrients for feeding. A normal, healthy GI tract is covered with a protective mucous layer, but this layer is damaged in leaky gut syndrome, IBD, and other inflammatory GI conditions. With damage to the lining, bacteria have even more opportunity to attach to the vast surface of the intestine and initiate biofilm construction.
Breaking Down Biofilm Is the First Step
In order to heal many modern-day infections, disruption of the biofilm is the necessary first step. Enzymes such as nattokinase and lumbrokinase have been used extensively as coatings on implants to fight biofilms (3). Therapeutic use of these enzymes may also be effective for breaking down biofilms in the gut and nasal passages.
N-acetylcysteine (NAC) is an antioxidant enzyme and a precursor to glutathione. It has been shown to effectively fight against biofilms on prosthetic devices, in vitro biofilms, and in chronic respiratory infections. NAC is recognized as a “powerful molecule” against biofilms (4).
Lauricidin (other forms: monolaurin, lauric acid, and glycerol monolaurate) is a natural surfactant found in coconut oil that helps inhibit the development of biofilms. It is particularly useful with yeast/fungal and viral biofilms.
Cistus incanus, a perennial shrub plant with high polyphenol concentration, is an excellent biofilm buster, particularly in the presence of bacteria involved in Lyme disease. The plants are found on dry or rocky soils throughout the Mediterranean, from Morocco and Portugal through to the Middle East and the Canary Islands. Clean sourcing is critical for this plant, typically used in tea or tincture form. The antioxidant properties of cistus incanus are touted to boost skin and and oral health as well.
Moving the Pathogen
There is extensive research on the ever-increasing resistance of pathogens to antibiotics and antifungal medications. Many herbal remedies are being shown to be more effective than their pharmaceutical counterparts in protocols working with pathogens.
Herbal medicines are complex biological compounds that have evolved and adapted over millenia. Their multitudes of active compounds are created by nature to work together synergistically. Pharmaceutical medicines are designed to annihilate vs. work towards balance and the modulation of the immune response. Surely, we are seeing the effects of a long period in history now of utilizing annihilation tactics. It isn't working, and the bugs we have now are altering themselves to attack back.
I prefer to work inside the understanding that if the body is out of balance and hosting a pathogen, we want to "move" it, not annihilate it. Reminding our bodies of their innate wisdom and abilities to keep things in balance is an important part of healing.
Managing the Influx of Heavy Metals
Heavy metals are everywhere, and are a real modern-day problem. There is no way to completely avoid them, but there are a myriad of ways to manage their levels and to prevent the body from building such high levels that the body becomes a very tantalizing location for pathogens to reside. First and foremost in this vein is to educate oneself and adapt an ecologically-based lifestyle. Read here for more information. Next, individualized and adequate detoxification procedures are necessary for us all. Detox is a daily practice, not something we can do in a "kit" or once annually session. It is an ongoing need and must be handled in accordance with the body's capabilities and responsiveness. Binders can be a very safe and useful tool in the management of heavy metal toxicity. You may read more on this topic here
Feeding Your Body By Your Type
We are each a unique biochemical individual. No two people have the same needs in their daily nutrition, and no two people will heal the same way. It is very important for long-term stability and immune modulation to adapt a lifestyle of eating properly for your Metabolic Type®. All of your homeostatic mechanisms are served by MT, as well as your body's ability to produce ATP. ATP is the fuel for every one of your body's trillion cells, and it is generated from efficient, individualized nutrition. Food is not just calories, not just sustenance - it is information. It communicates with and instructs your DNA on what to do. Learning how to maximize its power with your unique needs is a lifelong gift that will support your immune modulation and detoxification patterns.
If you are struggling with pathogenic activity and need assistance with biofilm disruption and detoxification, please contact me at Julie@truenaturehealthconsulting.com. Together we will develop a program for your success and immune recovery. We provide holistic telehealth services.
SOURCES
1) Joshua L. Kennedy, M.D. and Larry Borish, M.D, Chronic rhinosinusitis and antibiotics: The good, the bad, and the ugly, American Journal of Rhinology and Allergy, 2013 Nov-Dec
2) Römling U1, Biofilm infections, their resilience to therapy and innovative treatment strategies, J Intern Med, 2012 Dec
3) Hogan S1, O'Gara JP2, Novel Treatment of Staphylococcus aureus Device-Related Infections Using Fibrinolytic Agents, Antimicrob Agents Chemother. 2018 Jan 25
4) Dinicola S, DeGrazia S, Carlomagno G, Pintucci JP, "N-acetylcysteine as powerful molecule to destroy bacterial biofilms. A systematic review", Eur Rev Med Pharamcol Sci, October 2014
4) Stephen Buhner, "Herbal Antibiotics: Natural Alternatives for Treating Drug-Resistant Bacteria"