The Lesser Known Causes of Histamine & Mast Cell Conditions
Hello, I am Julie Donaldson and I am a clinical nutritionist with functional health training. I specialize in restoring balance in complex, chronic and acute health conditions. I welcome you to peruse other articles that may be of interest to you in your health investigation!
“I worked for years with people who pushed low-histamine diets to solve my problems - it never worked with the exception of random days. Then Julie was recommended for me, and everything changed. I no longer have the bothersome symptoms I lived with for decades. Be patient! It takes piecing the puzzle together and getting to the synergy of it all. It’s worth it.”
The internet is teeming with information about histamine intolerance. Unfortunately, the bulk of it is superficial information suggesting that histamine excess and intolerance are caused by food, and that histamine is the problem - it is, rather, a byproduct of the problem. While food plays an aggravating role in an over activated system, it is not the cause. Here, we take a much deeper dive into histamine and mast cell activation. We’ll cover the thyroid, infections/parasites/mycotoxins, calcium regulation, ATP, mental/emotional stress and oxidative stress as major underlying root causes of these challenges.
Major symptoms of histamine intolerance
Below are the major symptoms of histamine intolerance and/or mast cell activation
Gastrointestinal Symptoms
Diarrhea and/or constipation
Bloating
Nausea or vomiting
Abdominal pain
Dermatological Symptoms
Flushing, burning or redness of the skin
Itching, hives or rash
Pins & needles sensation
Respiratory Symptoms
Nasal congestion
Shortness of breath
Asthma-like symptoms
Neurological Symptoms
Headaches or migraines
Light sensitivity
Dizziness
Fatigue
Insomnia
Pain/stiffness
Cardiovascular Symptoms
Irregular heart rate (arrhythmia)
Low or high blood pressure
Palpitations
Additional Symptoms
Food sensitivities
Difficulty regulating body temperature
Anxiety and/or mood disorders
This is a big list and as one can see, there can be a lot of overlap with numerous other conditions. It takes a high level of awareness to recognize a histamine/mast cell pattern in the body and to determine the root causes. Nearly all advice is focused on limiting high-histamine foods. Let’s talk about where this all stems from and what the true solutions are - it all begins with mast cells.
Mast cells release histamine
As one of the key components of the immune system, mast cells are well known for their role in allergic reactions. However, they are also involved in inflammatory and fibrotic processes. Mast cells participate in all the stages of acute inflammatory responses, playing an immunomodulatory role in both innate and adaptive immunity. Mast cell-derived histamine, TNF-α, and IL-6 contribute to the inflammatory processes, while IL-10 mediates the suppression of inflammation. Crosstalk between mast cells and other immune cells is also involved in the development of inflammation.
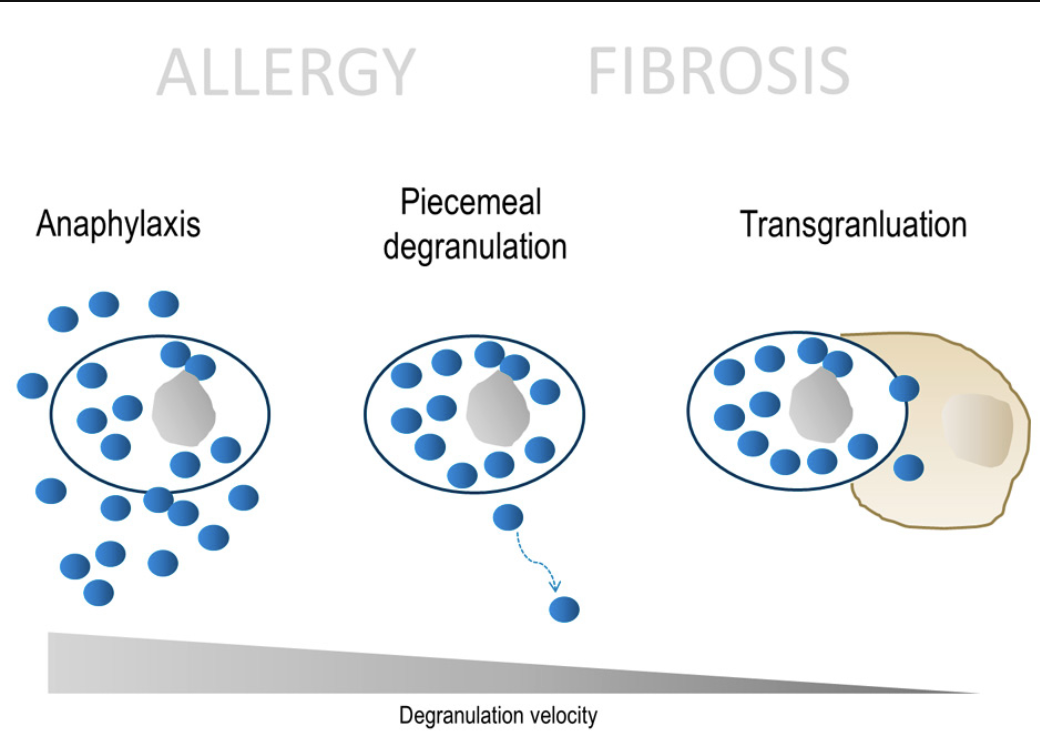
Mast cells degranulate. Degranulation is a cellular process that releases antimicrobial or cytotoxic molecules from within the mast cell. Degranulation in mast cells is part of an inflammatory response, and histamine is one of the substances released. Granules from mast cells mediate processes such as vasodilation, vascular homeostasis, innate and adaptive immune responses, angiogenesis, and venom detoxification. Especially in the case of a severe allergic reaction (1st image below), all of these releases and responses are appropriate and helpful in the body’s attempt to return to homeostasis. But in the event of ongoing pathogenic presentations and responses (2nd image below), the continued release and “transgranulation” into other body cells/tissues (3rd image below) of cells is a chronic inflammatory response which causes many of the symptoms listed above. It also causes fibrosis - fibrous, hardening of body tissues. The reactions of mast cells are not consistent for acute tissue injury vs. chronic tissue damage.
Mast cell degranulation and transgranulation
Distribution and impacts of mast cells
In addition to the connective tissue and mucosal tissues, mast cells are also located in many endocrine glands, including the hypothalamus, pineal, and pituitary glands. They are also found in the blood-brain barrier, peripheral nerves, the heart and arteries. Their adjacent location to multiple areas of the autonomic nervous system makes them of particular interest in conditions involving neurological symptoms - this is rarely anything discussed or investigated by medical practitioners. The problem didn’t start in the nervous system, it started in the immune cells nearby. Nerve endings have receptors for mast cell mediators, including histamine.
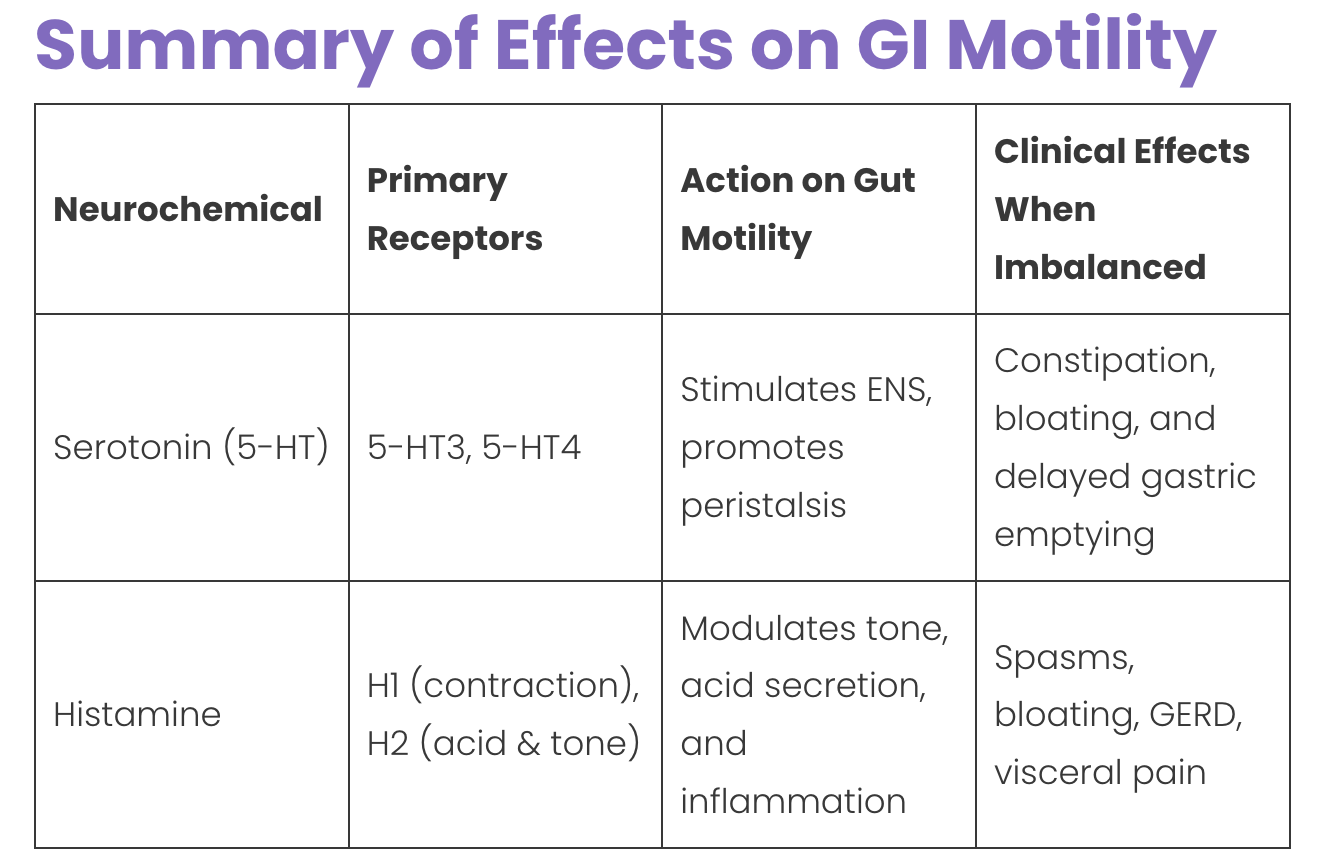
Your gut is mucosal tissue and thus has mast cells. That is a good thing under normal circumstances - again, not when chronically activated. Histamine is a regulator of the muscle activity in the gut. When it is out of balance in the gut (often due to dysbiosis), the firing of signals for the gut to contract & relax is changed. What happens? anything can happen - diarrhea, constipation, gas & bloating are the most common responses. The muscles are confused. Infections like H pylori as well as milder pathogenic conditions can completely disrupt normal gut motility.
Histamine and gut motility
What does all of this mean? While gut healing matters, mast cells and histamine imbalances are a complex picture, and until all of the pieces are addressed, the gut will not respond as it is designed to until the whole terrain is stabilized.
Another critical piece is that of ATP production and the redox system. This is a regular conversation here at True Nature, and it is one with far-reaching impacts that also involve vitamin D and VDR activation. When ATP production is compromised, mast cell behavior is likely to change.
The thyroid connects directly to this scenario as well. Balanced thyroid activity requires adequate ATP and simultaneously, the mitochondria (where ATP is produced) rely directly upon thyroid hormone modulation.
The relationship between the thyroid and mast cells is certainly complex and likely two-fold. There is evidence that T3 effects can be modulated by mast cells, and that mast cells can modulate thyroid function. Hyperthyroidism increases ATP production but simultaneously speeds up ATP hydrolysis (consumption) and causes mitochondrial inefficiency. Hyperthyroid activity also induces tissue damage and mitochondrial damage. There is evidence that T3 effects can be modulated by mast cells, and that mast cells can lead to excessive ATP production, higher energy turnover, increased heat production, and often, overall energy depletion. This is why people with hyperthyroid tendencies often have chronic issues with bloating caused by mast cell activity in the gut. Secondarily, thyroid hormones help to regulate calcium & phosphate levels in the body. Specialized ATP-dependent transport proteins called plasma-membrane calcium pumps regulate intra and extracellular calcium. What happens when this doesn’t occur? Calcium imbalances incite mast cell activation. Specific calcium channels, when imbalanced, may fail to control what’s called the zinc wave in the body. Zinc helps to modulate mast cell activity and is released from inside cells in response to their presence.
Oxidative stress also affects calcium signaling. Can you see how incredibly linked all of these functions are? One cannot address histamine & mast cell issues in a vacuum. A major contributor to oxidative stress (in addition to pathogens, VDR deactivation & mitchondrial stress) are heavy metals. Heavy metal accumulation in the body also interferes with mineral absorption, inclusive of calcium.
Psychological stress impacts mast cell activation as well, primarily via the gut-brain axis. Research continues to investigate suggested neuroimmune connections between stress-mediated mast cell activation and the development of neurological diseases. CRH activation of mast cells, potential disruption of the blood-brain barrier, intestinal permeability, and neuroinflammation are some of the components recently evaluated in this complex, multisystem relationship. CRH Is a hormone produced in the hypothalamus that acts as the primary driver of the body’s stress response, triggering the release of adrenocorticotropic hormone (ACTH) from the pituitary gland to increase cortisol. When stress is high, mast cell activity & histamine release activate CRH, which in turn activates the release of cortisol, our stress hormone. Both cortisol and histamine are “alert signals” in brain neurotransmission. A rise in cortisol when adenosine triphosphate (ATP) levels are low is a critical physiological response aimed at restoring cellular energy balance, often triggered by stress, fasting, or hypoglycemia. Cortisol functions as a catabolic hormone that mobilizes stored energy resources (glucose, fatty acids, amino acids) to increase ATP production when the body perceives a metabolic crisis. When a person focuses on lowering histamine vs. addressing the root cause of its elevation, natural responsive mechanisms that are designed to re-balance the body are being diminished. Alert signals and stress hormones have a purpose in our physiology.
The good news of natural supports
There is good news when it comes to natural mediation of mast cell activation & histamine intolerance. First, we must understand root causes to make the right applications. But, below is a list of potential mediators to be considered:
Histamine-lowering probiotics (which work in conjunction with butyrate)
Flavanoids, ECGC, terpenoids (from CBD), ellagic acid, resveratrol, curcumin & theanine
And remember something we discuss regularly and test for here at True Nature…histamine is degraded in the methylation processes by the HMNT and DAO enzymes. If those processes are not working properly, histamine will accumulate even in spite of mast cell activity.
Summations and solutions
Summing up, mast cell activity is affected by all of the following root causes:
Poor ATP production and/or rate of synthesis
Imbalanced thyroid activity
Calcium imbalances crucial to electrical stability
Dysbiosis, impaired gut barrier and/or presence of pathogens such as bacteria, parasites & mold/mycotoxins
Oxidative stress
Heavy metal accumulation
Under or over methylation
Low vitamin D and/or VDR activation
Mental/emotional stress
We don’t discuss problems without solutions at True Nature. We also don’t simplify solutions to the point of ineffectiveness. But what we will do is carefully determine what’s causing your problem and work with you to correct it.
In addition to investigating all of the above, we will ensure that you have individual, appropriate approaches to address any areas of concern. Your nutrition will be personalized, as will your testing, protocols and nervous system/stress practices. Please contact me at Julie@truenaturehealthconsulting.com for more information.